Learn the definition of myasthenia gravis (MG), an explanation of how it works and more information.
Myasthenia gravis (my-us-THEE-nee-uh GRAH-vis), sometimes called MG, is a rare autoimmune, neuromuscular condition that causes muscle weakness and fatigue.1 In fact, the name literally means “serious muscle weakness,” which is the primary symptom.2 There are two main categories for symptoms of MG: ocular and generalized. Ocular MG affects the muscles controlling the eyes and eyelids.3 Generalized MG (gMG) can affect muscles throughout the body.1
There are different types of MG—the most common type is called anti-AChR antibody positive gMG, which accounts for about 85% of people who are living with MG.4 To understand why these symptoms occur, it’s important to learn about the neuromuscular junction and the immune system.
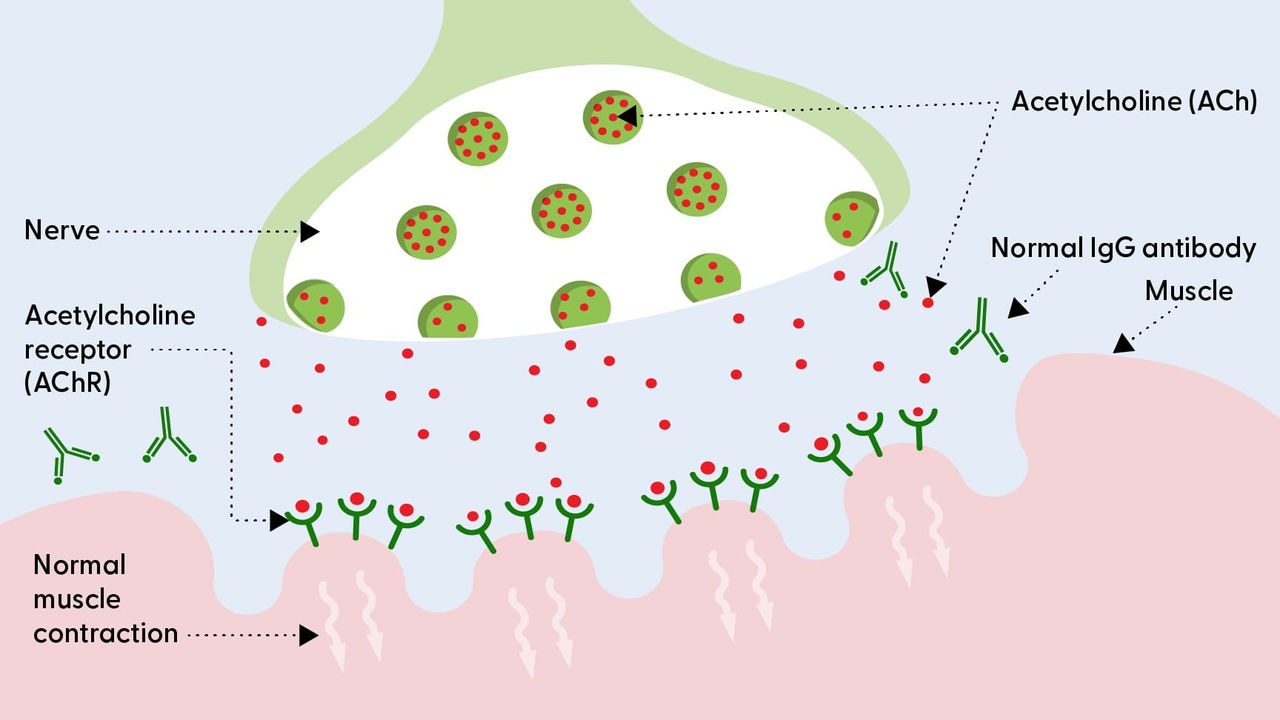
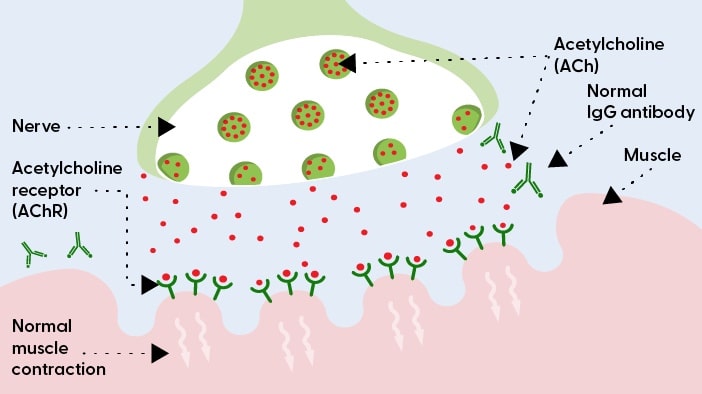
The neuromuscular junction without MG
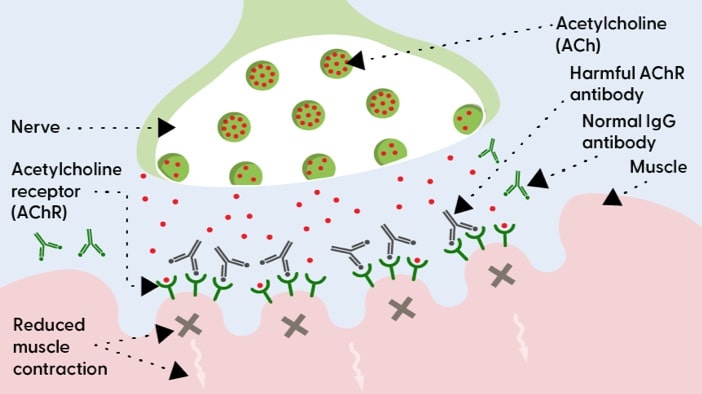
The neuromuscular junction is an area between the nerve and muscle, and it’s the part of the body where the brain tells the muscle to move. The brain uses the nerve to send messages called acetylcholine (ACh), which travel across the neuromuscular junction to the muscle. The muscle receives these messages using acetylcholine receptors (AChR).5
MG is an autoimmune disease. An autoimmune disease means that the immune system, which normally protects the body, is accidentally hurting it.5 Antibodies, or immunoglobulins (Ig), are proteins the immune system creates to fight infection and disease.6 The immune system makes five types of antibodies.6 Immunoglobulin G (IgG) is the most common of the five antibodies, and the one that plays a role in MG.7
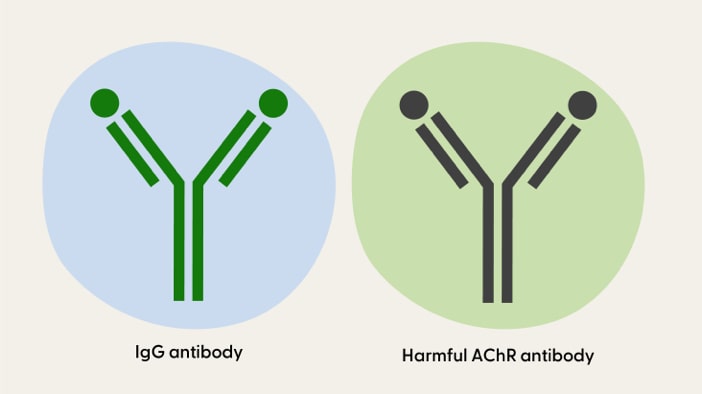
IgG antibody and harmful AChR antibody
In anti-AChR antibody positive gMG, the immune system accidentally creates antibodies called harmful AChR antibodies that attach to the AChR (receptors) in the neuromuscular junction. MG symptoms occur when these harmful AChR antibodies attach to AChR.7
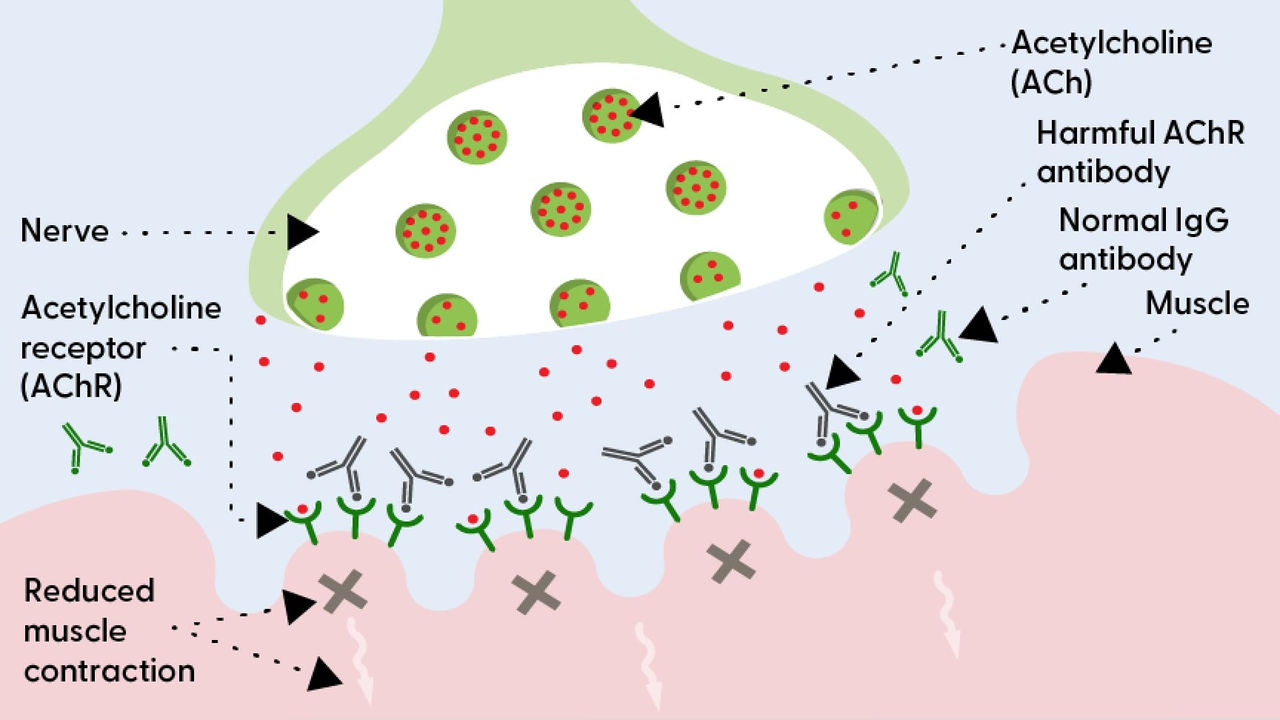
The neuromuscular junction with MG
When harmful AChR antibodies attach to AChR, they block, damage, or destroy the AChR, which interrupts nerve-muscle communication. This prevents the muscles from getting some of the messages sent by the nerves, leading to MG symptoms.8
MG is a serious disease. If you are diagnosed with MG, you may want to track your symptoms and talk to your doctor about your symptoms and treatment options.
While there is no cure, MG symptoms can be treated. A treatment goal for people living with MG is to reduce symptoms or become symptom-free for a period of time. People may experience minimal symptom expression (MSE), meaning they score 0 or 1 on the MG-ADL scale.9 The MG-ADL scale is one tool used to measure MG symptoms, where symptoms are measured from 0-24, with a higher score meaning more severe MG.10 You may want to have frequent conversations with your doctor about your MG symptoms.
Some MG symptoms include5,11,12:
- Eyelid drooping
- Blurred or double vision
- Difficulty speaking
- Difficulty chewing/swallowing
- Difficulty supporting neck
- Shortness of breath/difficulty breathing
- Weakness in the arms and legs
- Difficulty walking/standing
- Fatigue from repeated muscle use
Those with MG can lead happy and productive lives. There is a lot to learn, and there are many challenges. You can learn more about the treatment landscape for MG as well as the various community advocacy organizations of people living with MG. There are doctors and supporters who want to help make living with MG better.
We are part of that community and want you to be, too.
Fast facts
- There are six types of MG: generalized MG, ocular MG, seronegative MG, congenital MG, juvenile MG and transient neonatal MG1,13-15
- MG is not genetic (inherited), and it’s not contagious2,16,17
- MG affects people of all ages and races, but it is slightly more common in women 20 to 30 years old and men 50 to 60 years old18
- MG is a rare disease. An estimated 10,334 Canadians are living with it19, 20
MG glossary:
When it comes to having MG, knowledge really is power. Here are a few medical terms that people living with MG or supporting someone with MG may find helpful.21-23
- Acetylcholine (ACh): a compound that occurs naturally in the body and helps nerves communicate with muscles
- Acetylcholine receptors (AChR): help muscles receive acetylcholine signals from nerves
- AChR antibody: antibody that binds to acetylcholine receptors
- Autoimmune disease: the immune system mistakenly attacks the body’s own cells and tissues
- Diplopia: double vision
- Dysphonia: voice disorder
- Dysarthria: slurred speech
- Dysphagia: difficulty swallowing
- Exacerbation: also known as flare-up, symptoms increase in frequency and/or become more severe
- LRP4: stands for low-density lipoprotein receptor-related protein 4. Like ACh, it’s a protein that helps nerves communicate with muscles
- MuSK: stands for muscle-specific kinase
- MuSK receptor: like ACh, it’s a protein that helps nerves communicate properly with muscles
- MuSK antibody: antibodies that bind to the MuSK protein
- Myasthenic crisis: worsening of myasthenic weakness requiring intubation or noninvasive ventilation to avoid intubation
- Neuromuscular junction: site of communication between motor nerves and muscle fibers that makes muscles work properly
- Ptosis: drooping eyelids
- Seronegative myasthenia gravis: a form of MG in which autoantibodies are not detectable in the blood
- Thymus: the thymus is an organ that's part of the immune system
- Thymectomy: a surgery to remove the thymus